Treatments – Anus
Anal fissure treatments
The treatments for anal fissure aim to break the cycle of hard bowel motion, pain and sphincter spasm. Increasing the fibre in your diet and using some warm baths for 15min a few times a day (Sitz bath) may sometimes be enough to heal your fissure. Local cream preparations which relax the anal sphincter in combination with laxatives can also be used. If these fail then a step wise approach of the treatments options below may be followed until the fissure heals.
Injection of reversible Neurotoxin +/- fissurectomy
Neurotoxin injection can be used for treatment of conditions such as anal fissure, anismus or chronic pelvic floor pain. Neurotoxin is widely known as a safe and effective cosmetic treatment. This procedure is performed under general or regional (spinal) anaesthesia as a day procedure. When used for anal fissure treatment it is also called chemical sphincterotomy. It involves cleaning the tissue around the fissure area down to fresh tissue (fissurectomy) and the injection of neurotoxin into the anal sphincter. This leads to relaxation of the sphincter which then allows enough blood supply to reach the inner lining area and heal the fissure. The beneficial effect of the neurotoxin starts appearing at approximately 2 weeks with the full effect is felt at 6 weeks. The overall effect of the neurotoxin lasts approximately for three months.
This is a very safe procedure which can be repeated if required. Specific risks of the procedure include rare medication allergy to the neurotoxin and a risk of temporary flatus incontinence. Roughly 50-60% of patients get better with one course of treatment. One of the main benefits of this procedure is the avoidance of the risk of permanent incontinence which comes with the lateral sphincterotomy procedure.
Lateral sphincterotomy
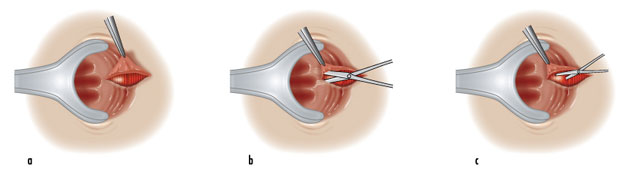
Lateral sphincterotomy is a procedure performed under a general or regional (spinal) anaesthetic as a day procedure. The procedure itself takes 20 minutes and involves permanently dividing a part of the anal sphincter which leads to loss of power of the sphincter, improved blood supply and healing of the fissure. It has the best success rates in terms of healing rates (95%) for the fissure but comes with a small risk of permanent incontinence to flatus or faeces (5%) which may lead to some minor soiling of the underwear. The risk of incontinence makes this procedure the last resort in terms of treatment options for anal fissures.
Anal advancement flap
This procedure is reserved for patients that have been found to have an anal fissure but with a weak anal sphincter. Further division of the sphincter with lateral sphincterotomy would not be effective in these cases. The procedure involves a general or regional (spinal) anaesthetic and takes place as a day procedure. An enema may be given to you on the day to clear your bowel. The operation lasts for approximately 60 minutes. It involves the creation of a flap of healthy skin or lining of the bowel with a rich blood supply which is moved and sutured over the fissure area in order to heal the fissure.
Specific risk to this procedure involves the wound opening up and a wound developing. It is thus important to avoid sitting on the wound for 2 weeks until you are seen in clinic. If you are worried about the wound opening please let my office know. The success rate is approximately 60%.
Recovery
After the procedure you will wake up in a hospital room. All of the above procedures are normally performed as day case operations but sometimes patients may need to spend a night in hospital. You are typically expected to go home once you are eating and drinking, are able to manage the pain and walk unaided and have passed some urine. You will be prescribed some pain killers to go home with and you will need to use laxatives for at least 4 weeks after the procedure and try and keep your motions soft. It normally takes about 2 to 4 weeks to fully recover from the anal advancement flap procedure and return back to work and 1-2 weeks from the other procedures, but it varies from person to person and depends on their general health and the nature of their work.
Risks of procedures
All of the above procedures carry a similar risk to complications as other procedures. These include complications common to all surgical procedures such as infection, bleeding, blood clots, heart problems, pneumonia, urinary retention, anaesthetic risks.
Need to contact us or book an appointment?
Disclaimer
The information relating to general and colorectal disorders and their treatments given on this website is not complete and is not intended as a substitute for a consultation with your doctor. Always seek medical advice from your doctor before making a decision about any of the conditions and/or treatments mentioned on this website.
© Dr Georgios Markides
Contact Information
You can always contact our Clinic for booking appointments and other useful information:
Dr. Georgios Markides,
Consultant General & Colorectal Surgeon
APEX Building, 47 Andreas Avraamides Str., 2024 Strovolos, Nicosia, Cyprus
+357-22-282008
